La 7e Journée universitaire du Département de radiologie, radio-oncologie et médecine nucléaire de la Faculté de médecine de l’Université de Montréal a eu lieu le 21 février 2019 à l’agora du Centre de recherche du CHUM. Trois étudiants ont reçu un prix pour leur présentation.
Premier prix – Présentation scientifique orale par un étudiant
Récipiendaire
Marie Amate
Titre de la présentation
Cancer Immunotherapy: Enhanced monoclonal antibody (mAb) delivery using microbubble and ultrasound treatment
Équipe
Marie Amate 1,2, Balasubramanian Sellamuthu 2, John Stagg and Francois Yu 2
Affiliations
Université de Technologie de Compiègne 1, Université de Montréal (CRCHUM) 2
Résumé
Introduction. The tumoral microenvironment is characterized by a high interstitial pressure which forms a physical barrier to the diffusion of drugs from the vasculature into the cancerous stromal space. This is an especially challenging hurdle for large molecules, such as antibodies. Thus, the primary objective of this study is to improve immunotherapy by helping monoclonal antibody distribution into solid tumors by microbubbles (MB) and ultrasound (US). Here we present enhanced anti-CD73 (mAb) delivery to a tumor using optimized MB+US treatment.
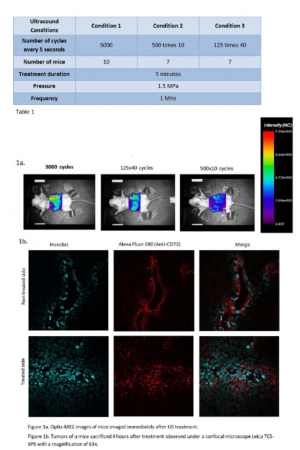
Methodology. This study was conducted in female Balb/c mice bearing bilateral subcutaneous 4T1 breast cancer tumors (≈250 mm3 in 2 weeks with an injection of 106 cells). A bolus of Alexa- Fluor 680 labelled antibodies (100μg) were injected by the tail vein. Definity microbubbles (150μL) were injected intravenously at the speed of 4μL/min during US treatment. The right side was subjected to US (tested on three cohorts of 6-9 mice) using three different ultrasound conditions (Table-1) while the left side served as a paired non treated control. After treatment, mAb distribution was assessed using an optical fluorescence imager (Art Optix-MX2, GE). After US-treatment 600μg of Hoechst33342 was injected intravenously (vascular stain) and mice were sacrificed humanely to collect tumors for histology.
Results and Conclusion. In US treated tumors with 5000 cycles pulses, fluorescence was increased compared to the control side. Confocal microscopy corroborated the findings, as mAb could be found penetrating away from the vessels in the treated tumor whereas they remained restricted to the vascular space in the non-treated tumors.